Review of Paul Hodges talk on Motor Control, Part One
This is part one of my review* of Paul Hodges’ talk at the conference on pain and motor control that he did with Lorimer Moseley in Portland in October 2012. You can read my review of Lorimer’s talk here.
Professor Transversus Abdominis
 Hodges is a professor of physiotherapy and neuroscience at the University of Queensland in Australia. Since the 1990s, he has done a significant amount of research exploring the muscle activation patterns of people with back pain. Yes, he is the guy who found that people with back pain tend to use their transversus abdominis (TVA) a little differently than people who are pain free. He did the research that launched a million abdominal draw ins!
Hodges is a professor of physiotherapy and neuroscience at the University of Queensland in Australia. Since the 1990s, he has done a significant amount of research exploring the muscle activation patterns of people with back pain. Yes, he is the guy who found that people with back pain tend to use their transversus abdominis (TVA) a little differently than people who are pain free. He did the research that launched a million abdominal draw ins!
And Hodges seems acutely aware that many people have really misinterpreted his research. His talk spent almost as much time trying to correct the misconceptions as explaining what he actually found.
So it was great to hear a perspective on core stabilization from the guy who did a lot of the pertinent research. He came off as a very careful thinker. Here’s a guy who has been studying a very focused issue for a very long time, has learned a great deal of fascinating information, and is still very ready to admit there is still so much we don’t know about the relationship between motor control and pain.
The connection between the two presentations
Interestingly, Moseley started his PhD under Hodge’s supervision, and they have apparently remained in close contact since then. So they are very aware of one another’s work, and each referred to the other several times in their presentations. Even though these guys have often been pointing their microscopes in different directions over the years, they both know that they are only looking at pieces of the larger puzzle.
So how do the pain and motor control pieces fit together? Although’s Hodge’s presentation was separate from Moseley’s, there was some cross over. For example, Moseley talked about how threatening inputs can induce motor control changes. For example, stiffening certain muscles might protect against movements that are considered to be dangerous.
And Paul discussed in great detail the exact nature of the motor control changes that are found in the presence of pain, particularly in the area of the torso and the pelvic floor. He also talked (a little less) about how motor control problems might cause pain, and how such problems can be identified and remedied to help treat pain. Please note that these are all separate issues. In this post I will talk about Hodge's discussion of how the spine is optimally stabilized from a mechanical standpoint. Try to remember that the issue of whether or not suboptimal stabilization strategies cause pain is a separate question which I will address in a later post.
Spinal control
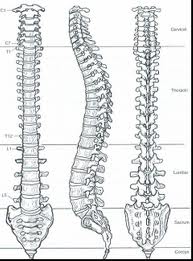 Although Hodges’ talk was titled motor control, its primary focus was control of the spine, particularly stabilization. A spine is hard to stabilize because it is basically twenty four hockey pucks stacked vertically with a bowling ball at the top. No, Hodges did not offer that image at the presentation. I made up that nonsense all on my own!
Although Hodges’ talk was titled motor control, its primary focus was control of the spine, particularly stabilization. A spine is hard to stabilize because it is basically twenty four hockey pucks stacked vertically with a bowling ball at the top. No, Hodges did not offer that image at the presentation. I made up that nonsense all on my own!
One key to stabilizing the spine is to avoid buckling, which means the whole stack falls down. Another goal is maintaining segmental control, which means preventing any individual vertebrae from sliding too far from its neighbor. If the spine buckles or loses segmental control, this can impair function, cause loss of balance, and/or damage to tissues around the spine.
Spinal stabilization is not just for heavy deadlifts, it needs to happen all day long. Any movement of the arms or legs will create forces that will tend to cause buckling or shearing of the spine unless the core muscles take action to maintain proper alignment.
And spinal control is not just about preventing unwanted movement, it is also about creating useful movements. For example, changing the orientation of the spine (e.g. vertical, horizontal, extended, flexed) facilitates movement of the head and limbs, breathing, shock absorption, transmission of forces, and maintenance of the center of gravity over the base of support.
So how do we control the spine?
Muscular division of labor
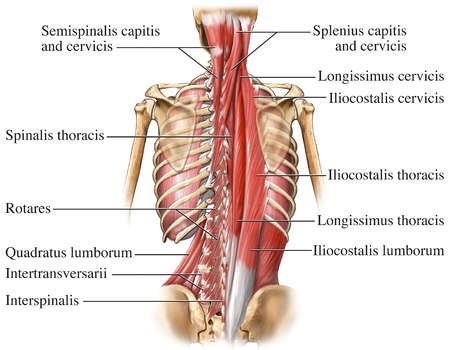 Hodges’ analysis of core stabilization includes the familiar concept of distinguishing between deep local muscles that perform a stability function and superficial global muscles that provide more of a movement function. Some have objected to this distinction on the basis that all muscles can perform either function depending on the circumstance, so we can never say that one muscle is purely a stabilizer and another is purely a prime mover. That is true, but the distinction between global and local muscles definitely has some logic, and is based on considerable anatomical and functional evidence, as discussed below.
Hodges’ analysis of core stabilization includes the familiar concept of distinguishing between deep local muscles that perform a stability function and superficial global muscles that provide more of a movement function. Some have objected to this distinction on the basis that all muscles can perform either function depending on the circumstance, so we can never say that one muscle is purely a stabilizer and another is purely a prime mover. That is true, but the distinction between global and local muscles definitely has some logic, and is based on considerable anatomical and functional evidence, as discussed below.
The local stabilizers
The local spinal muscles lie deep in the body and cross only one or a few vertebrae, and are therefore well situated to provide intersegmental control of small movements of the vertebrae. Their placement also means that they have short moment arms, and are unable create powerful larger movements of the spine.
Some obvious choices for muscles in the local stabilizer category are the multifidus, intertransversarii, and transversus abdominis (TVA). For example, the deep fibers of the multifidus have a very limited ability to extend the spine, but can effectively compress vertebrae together to prevent undesired movements, particularly anterior translation.
The TVA, the most famous muscle in the local group, has only a minimal ability to move the spine, but is well positioned to tense the lumbodorsal facia and help create intra abdominal pressure (IAP), each of which can help compress the vertebrae and restrict intervertebral motion.
The psoas and the quadratus lumborum are not often considered as local stabilizers of the spine, but that is probably because it is very difficult to obtain EMG readings of their activity without some rather invasive techniques. But their placement (particularly the anterior fibers of the psoas and the medial fibers of the QL) suggest a strong ability to provide intersegmental control of the spine. Hodges said that one might even think of the psoas as an anterior multifidus, well suited to prevent posterior translation of the vertebrae.
The global movers
Unlike the locals, global muscles are more superficial, cross several joints, and therefore have large moment arms on the spine. Their placement means that they are not very good at controlling individual spinal segments, but very good at creating the torque necessary for large movements of the spine.
Muscles in this category include the rectus abdominis, the external oblique, the thoracic portions of the longissimus and iliocostalis and the anterior fibers of the latissimus dorsi. Although the global muscles can stabilize the spine through co contraction and compression, they do not have the fine tuned and nuanced control of the local muscles in doing so.
Global versus local: EMG analysis
Research shows that the global and local muscles actually behave differently in functional activities. When the spine is met with forces caused by walking or moving the arms, EMG analysis shows that the global muscles tend to act only when a specific direction of force is applied, and the local muscles activate regardless of the direction of force. So the activity of the locals is said to be tonic, and the activity of the globals is said to be phasic.
For example, the superficial flexors such as rectus abdominis will become active in anticipation of the need to flex the spine or prevent extension, but will be silent in the opposite case of extending or preventing flexion. By contrast, the TVA and multifidus will become active regardless of the direction of the force. Thus, the superficial muscles control the gross orientation of the spine (whether it is extended, flexed, vertical or horizontal, etc.) while the deep muscles provide control of the individual segments of the spine (whether one particular vertebrae is sliding one way or the too far forward or back of the line of the spine.)
Given the different talents of the core muscles, optimal stabilization requires that each muscle perform the role to which it is best suited. As I will discuss in the next post, one of Hodge's interesting research findings is that people in chronic pain tend to experience disturbances in the natural division of labor between the global and local stabilizers.
Breathing continence, and intra abdominal pressure
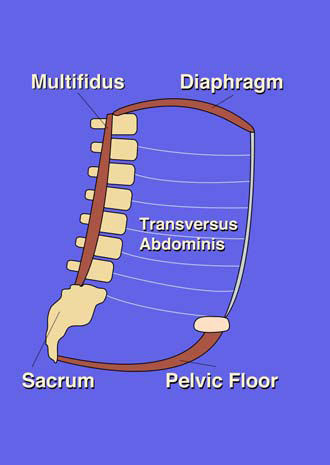 Another important component of spinal stability is provided by the dynamic interaction between the diaphragm, the pelvic floor, the TVA and lumbodorsal fascia. These structures form the four walls of the “abdominal cannister.” The right balance of activity between the muscles making up the four walls can modulate intra abdominal pressure (IAP) and therefore the stiffness of the spine. This balance will also affect breathing, movement ability, and continence.
Another important component of spinal stability is provided by the dynamic interaction between the diaphragm, the pelvic floor, the TVA and lumbodorsal fascia. These structures form the four walls of the “abdominal cannister.” The right balance of activity between the muscles making up the four walls can modulate intra abdominal pressure (IAP) and therefore the stiffness of the spine. This balance will also affect breathing, movement ability, and continence.
For example, breath holding increases IAP and tends to prioritize stability over respiration. This is why weightlifters hold their breath with a valsalva maneuver to elevate IAP and stiffness of the spine. And here’s something I didn't know. Hodges said that top sprinters will often run 100 meters without one inhale. Huh? If I can learn to hold my breath for twenty seconds I should give that a try.
It should also be noted that increased IAP elevates the demand on the pelvic floor muscles to remain continent. (Yes, a valsalva helps you poop.) Anyway, one of the points here is that the interrelated mechanics of the four walls of the cannister implies that there is a fine balance, and some tradeoffs between breathing, continence and postural control. Different activities will prioritize one function over the other, and this balance can be thrown off a little in people with chronic pain.
Timing
One important feature of core stabilization is that the muscular activity which creates it must precede any forces that tend to disturb the spine. So timing, anticipation and feedforward muscular activity are at issue. Many prominent movements experts including Vladimir Janda and Gray Cook have claimed that optimal stabilizer function is more about timing than strength. As discussed later, Hodges has some interesting research showing that people with pain tend to have timing issues with their local stabilizers.
Stability involves movement
Optimal stabilization of the spine is not just about preventing movement. Hodges' research shows that the most efficient strategy for stabilizing the spine is often movement, as opposed to rigid stiffness. Disturbance to the spine is less when the preparation involves an adjustment of the position of the spine. Thus stability is not just about preventing movement, it often involves subtle small movements made at the right time in the right amount. And yes, you guessed it, people with chronic back pain tend to use less movement in their stabilization strategies than people without.
More is not better
Hodges made the point repeatedly that optimal stablity is not about generating maximum stiffness and rigidity, but instead about contracting the right muscles, in the right amount, at the right time. Remember that the muscular contractions that stablize the spine are not without cost - they restrict breathing and movement, exert pressure on the pelvic floor, and increase compression of the spine. So more is not better, and the goal is instead balance, skill, and the ability to employ the right strategy at the right time.
Ok, that's it for now. In the next post I will try to discuss Hodges' extensive research on how optimal stabilization tends to be disturbed in people with chronic pain. Oh, and until then please don't go assuming that the dysfunction is causing the pain. Instead, it seems to be the reverse. Stay tuned.
